What’s Up With Endometriosis? The Low‑down You’ll Love
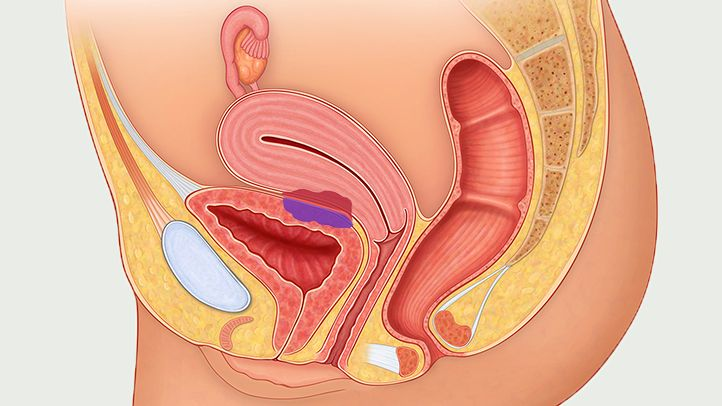
Picture this: a part of your uterus that usually keeps your cycles tidy decides to throw a party outside its usual spot. That’s endometriosis in a nutshell – a condition where uterine lining (the endometrium) gets a wild detour and starts nesting on ovaries, fallopian tubes, and other pelvic organs. Result? Pain, swelling, and all the drama of a tissues party that never gets the RSVP.
Why Should You Care?
India’s Endometriosis Society says about 25 million women (2.5 crore) are living with this obstinate problem. It can mess with fertility, turn everyday periods into an Olympic track of cramps, and sometimes lead to scary complications such as ovarian cancer.
The Three “Looks” of the Party
- Superficial peritoneal lesions – just scratching the surface.
- Endometrioma (ovarian lesion) – a cyst that’s basically a backstage festival.
- Deeply infiltrating – the most persistent guests that cut deeper into tissues.
What’s the Root? (or where It Started)
There’s no single culprit, but a popular theory is retrograde menstruation – menstrual blood flowing backward through the fallopian tubes, depositing stray endometrial cells in the pelvis instead of exiting the body. Think of it like a misdirected mail delivery that “sticks” around.
Under estrogen’s influence, the uterine lining thickens and, if pregnancy doesn’t happen, it breaks down and sheds. When it gathers in the wrong places, it stirs up irritation, inflammation, scarring, and sometimes a chain reaction of adhesions – all the drama that makes endometriosis a hard‑to‑ignore case.
Typical Symptoms (and Some “Drama”)
Below are common complaints, though reactions vary from “I can barely feel it” to “my bones are falling apart.”
- Intense periods and head‑butting cramps.
- Back pain swooping in during menstruation.
- Stiffness while peeing or pooping.
- Heavier bleeding or spotting.
- Blood mixed with stool or urine (we’re not kidding).
- Diarrhea or constipation.
- Sensitivity during intercourse.
- Persistent fatigue that refuses to go away.
- Difficulty getting pregnant.
Risk Factors – The “When You’re In Trouble” List
Early first periods, late menopause, lack of childbirth, and a family history all load the odds of catching this condition. A clutter of heavy periods, long flow, and high estrogen levels also play a part.
Most Common Complications
- Infertility – up to 50 % of women grapple with pregnancy.
- Rare cancers – including ovarian and endometriosis‑associated adenocarcinoma.
How Doctors Spot It
Diagnosis starts with a handful of symptoms, but confirmation often needs a combination of:
- Pelvic Examination – the doctor feels for lumps and scarring.
- Imaging (Ultrasound, MRI, CT) – looks inside the organs.
- Laparoscopy – the surgical “peep” with a camera to spot lesions.
- Biopsy – sampling tissue to give a definitive label.
Stages (ASRM’s Rating System)
From stage I (minimal) to stage IV (severe), the scale is based on lesion size, depth, and scarring.
Treatment Options: Pick Your Arsenal
Doctors usually start with conservative measures and move to surgical interventions if needed.
- Pain Relief – OTC NSAIDs like ibuprofen or Aleve tackle the cramps.
- Hormonal Therapy – lowers estrogen to stop periods and shrink lesions.
- Surgery – remove the heavy hitters; in extreme cases, a hysterectomy.
Lift Your Spirits and Look After Your Health
Remember, early diagnosis and timely treatment help you avoid the dreaded dance of infertility and late‑stage cancers. Couple that with a balanced diet, exercise, and stress management, and you’re already stepping toward a calmer, happier life. Extras like acupuncture, herbal remedies, or a gentle massage can help keep the negative vibes at bay.
Don’t let endometriosis be the ultimate party crasher – become the host that knows what’s happening inside and how to make that party a bit more well‑behaved.